Previous falls
Repeated incidents signal ongoing risk that should not rely only on scheduled rounds.
Patient bed alarms

Definition

Resident fit
Types of bed alarms




Sensor comparison
| Sensor type | Trigger point | Best for | Key limitation |
|---|---|---|---|
| Pressure pad | Weight lifts off pad | Single-room care, home settings | No location data; pad disrupted by linen changes |
| Early-alert | Resident shifts toward edge | High fall-risk residents, multi-bed wards | Requires correct pad positioning to stay accurate |
| Under-mattress | Pressure pattern changes pre-exit | Residents sensitive to contact; frequent linen changes | Higher cost than surface pads |
| Floor mat | Resident steps onto mat | Backup layer; low-risk notification | Triggers after exit - too late to prevent a fall |
Buying criteria
| Factor | Low-risk / home care setting | Higher-risk / care facility |
|---|---|---|
| Mobility & cognition | Mobile resident: pressure-pad or floor mat | Mobile + cognitively impaired: early-alert sensor |
| Environment | Audible alarm in client's home is enough | 20-30 residents per ward needs silent, routed alerts |
| Alert routing | Local audio or single-carer app | Device-specific alert with room and bed context |
| Monitoring type | Active: pendant or call button acceptable | Passive: pressure pad, under-mattress, or motion sensor |
Selection context




Feature checklist
Standalone vs connected
| Feature | Standalone alarm | Connected system (Guardian) |
|---|---|---|
| Alert destination | Audible beep at nurses' station | Named alert to caregiver's phone or tablet |
| Room and bed location | None | Room number and bed shown on floor plan |
| False alarm filtering | None | Configurable rules per resident and time of day |
| Response time log | None | Timestamped log with acknowledgement record |
| Incident documentation | Manual, paper-based | Dashboard with shift-level response data |
| Wireless range testing | Not applicable | Pilot available before full ward rollout |
Care-home reality

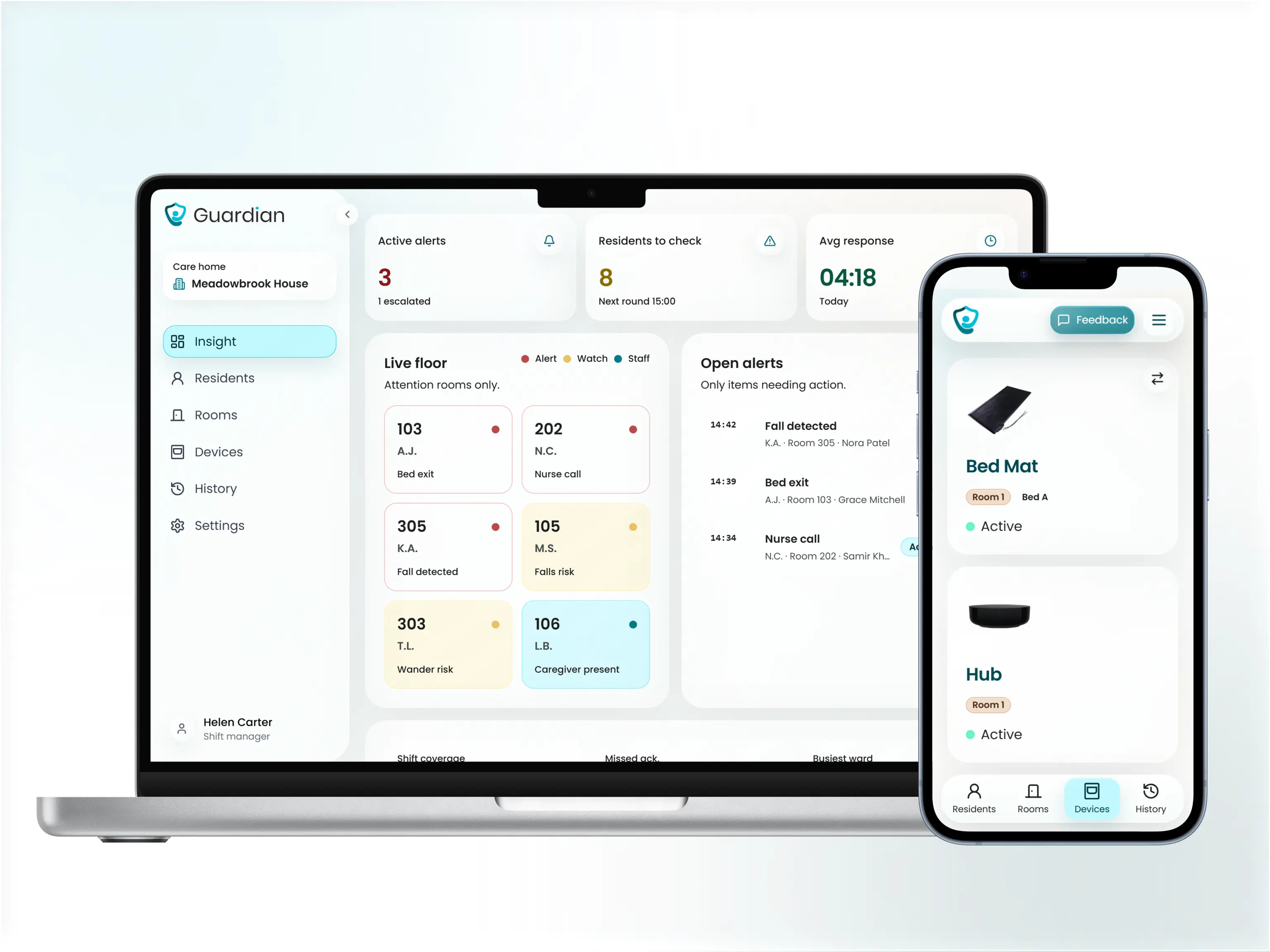
Guardian in care homes
Guardian in practice

Common questions
Move beyond standalone bed alarms