
Staff wristband
Shows each caregiver's live position on the floor plan, so alerts route to the nearest available person rather than broadcasting across the ward.
Caregiver alert systems

Definition
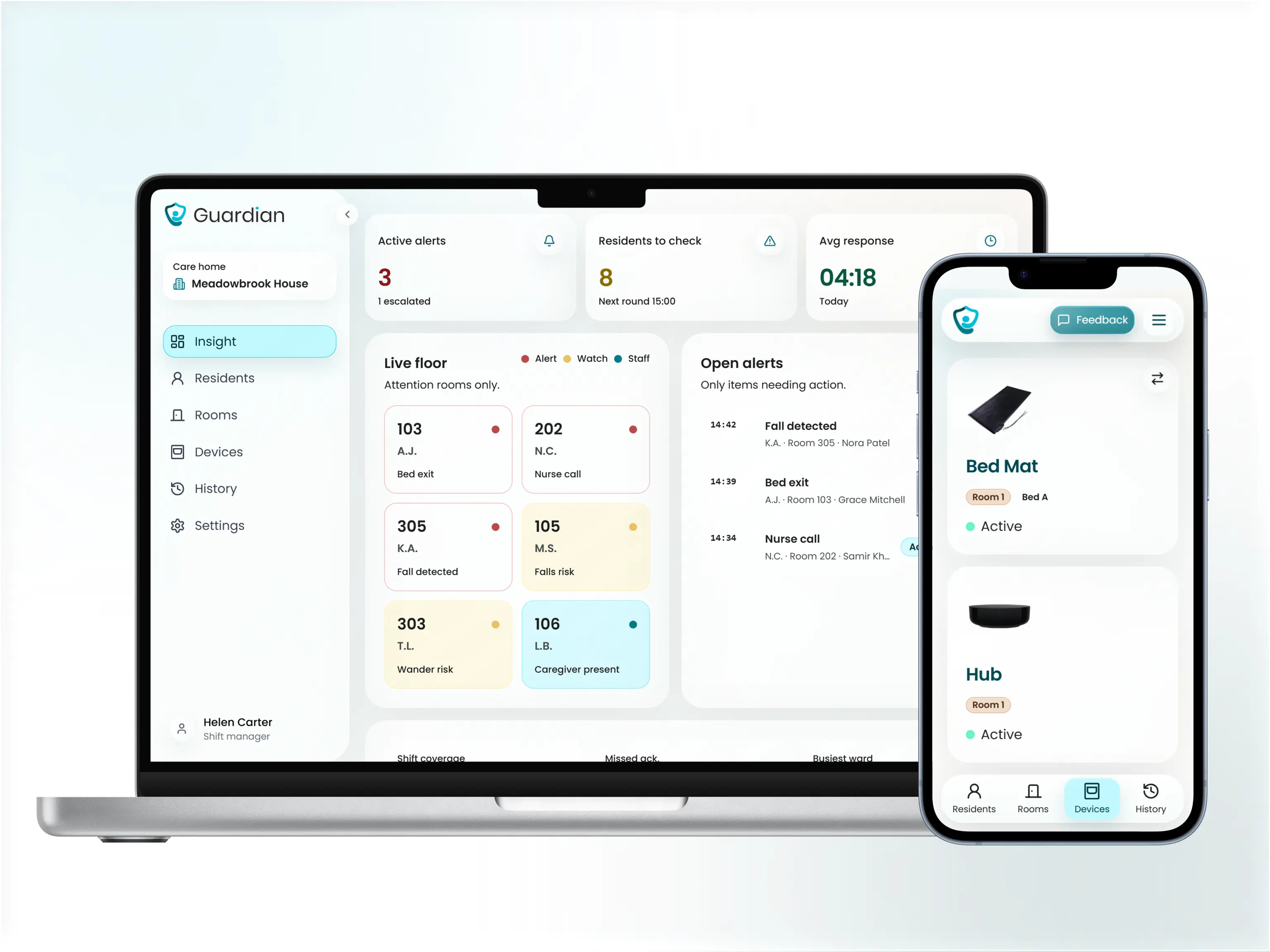
Device types



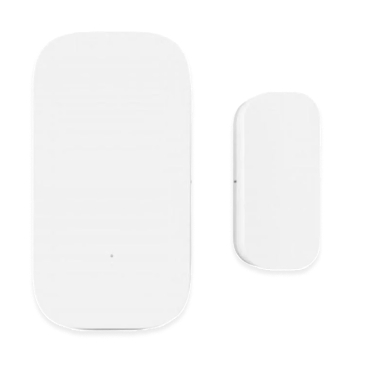
Device overview
| Device type | What it detects | Best used for | Alert type |
|---|---|---|---|
| Staff wristband | Live caregiver positions across the ward | Alert routing, coverage visibility, shift oversight | Real-time floor plan position, alert routed to nearest caregiver |
| Resident wristband (SOS + fall detection) | Manual SOS press and automatic falls via accelerometer | High fall-risk residents, including those who cannot press a button | Immediate alert with resident name and live room position on floor plan |
| Bed exit sensor | Resident leaving their bed | Fall-risk residents, especially at night | Instant targeted alert to nearest caregiver |
| Door sensor | Room or external door opening or closing | Wandering risk, room routine monitoring | Location-tagged alert mapped to floor plan |
Device detail

Device detail

Device detail

Device detail

Buying criteria
Guardian in care homes
Common questions
Pilot one ward first